AI in Healthcare: How Artificial Intelligence is Transforming Medicine in 2026
Artificial intelligence (AI) is automating healthcare workflow from end-to-end.
And for good reason: Physicians were spending more time staring at screens than at patients. A study in Annals of Internal Medicine found that physicians spend nearly 2 hours on EHR and desk work for every hour of direct patient care during office hours, plus an additional 1-2 hours nightly on EHR tasks outside work.
From ambient AI scribes that listen to patient visits and write clinical notes in real time, to machine learning algorithms that detect cancer in radiology images before a radiologist can, AI is moving from hype to hands-on clinical utility.
And it's moving at a pace that's hard to overstate. In 2024, the FDA cleared over 950 AI-enabled medical devices.
This guide breaks down what AI in healthcare actually means in 2026 — the technologies, the real-world applications, the benefits, the risks, and what clinicians and practice owners need to know before adopting any of it.
What is AI in healthcare?
Artificial intelligence in healthcare refers to the use of machine learning algorithms, natural language processing, computer vision, and related technologies to:
- Analyze clinical data
- Automate administrative tasks
- Support medical decision-making.
To be perfectly clear: none of these tools can or should replace physicians. They're designed to give back the cognitive bandwidth to do what only you can do: practice medicine.
Healthcare AI spans a wide range. There are chatbots that triage patient symptoms before a visit, eep learning models that flag early-stage diabetic retinopathy in a retinal scan, and ambient microphones that turn a physician-patient conversation into a structured SOAP note.
How AI processes clinical data
AI systems in healthcare are trained on large datasets — medical images, EHR records, clinical notes, genomic sequences, claims data — to identify patterns at scale. The process typically involves three stages:
- Data ingestion: Structured data (lab values, vitals, ICD codes) and unstructured data (clinical notes, imaging, voice recordings) are collected and formatted.
- Model training: Algorithms learn from labeled historical data. For example, thousands of chest X-rays annotated as "pneumonia" or "no finding."
- Inference: The trained model applies what it learned to new, real-world inputs and generates a prediction, recommendation, or output (like a clinical note).
The quality of an AI model is only as good as the data it's trained on — which is why bias, data privacy, and model transparency are central to every responsible healthcare AI deployment.
Key AI technologies used in medicine
Machine learning (ML)
This is the foundational layer of most healthcare AI. ML models find patterns in structured data — predicting which patients are at risk for sepsis, for example, based on lab trends and vital signs.
Natural language processing (NLP)
This enables AI to understand and generate human language. It powers ambient AI scribes that transcribe and structure clinical conversations, as well as tools that extract meaning from unstructured clinical notes.
Computer vision
This allows AI to interpret medical images — X-rays, MRIs, dermatology photos, pathology slides. Models trained on millions of annotated images can now match or exceed specialist-level performance in specific diagnostic tasks.
Generative AI
Now we have the technology behind tools like ChatGPT. It can synthesize, summarize, and generate text. In healthcare, it's being used to draft clinical notes, write after-visit summaries, and produce patient communication — though with important guardrails around accuracy and HIPAA compliance.
Key Applications of AI in Healthcare
When people hear “AI in healthcare,” they often imagine something futuristic — robotic surgeons or fully automated hospitals.
That's far removed from what clinicians actually need: help with the medical documentation, administrative work, and end-to-end workflows.
Here's how AI is making a positive mark for clinics and practitioners.
Clinical documentation and ambient AI scribing
Documentation burden is the highest-ROI application of AI in healthcare today. 77% of pulse survey respondents said that they finish work later than desired or work at home due to medical documentation.
Every patient visit requires clinicians to record key information including:
- Patient history
- Symptoms and exam findings
- Clinical impressions
- Treatment plans
- Follow-up instructions
This patient care documentation tool serves multiple purposes. It supports:
After-hours charting is so common that it's earned a name: "pajama time," ie., catching up on notes at 10 PM after a full day of patients. In fact, 63% of physicians in the US claim to be emotionally exhausted due to burnout.
Ambient AI scribes work by listening to the physician-patient conversation (with patient consent), transcribing it in real time, and generating a structured clinical note. The physician reviews, edits if needed, and approves. What used to take 15 minutes per patient takes two.
Freed's AI scribe, one of the leading ambient tools, supports 100+ specialties, and offers a one-click integration with browser-based EHRs such as athenahealth, eClinicalworks, Practice Fusion, Elation, and more. It also can:
- Carries patient context forward for continuity of care
- Surface ICD-10 and CPT codes with the highest possible E/M ratings
- Supports clinical-decision making with 50+ verified medical sources
- Generates patient letters, referrals, and any other documentation in several languages
.png)
See how Freed builds documentation, codes, and more.
Medical imaging and diagnostics
AI is arguably most mature in radiology and pathology.
FDA-cleared imaging AI tools now assist in reading chest X-rays, detecting breast cancer in mammograms, identifying strokes on CT scans, and flagging diabetic retinopathy in fundus photos.
In 2023, a landmark study published in Nature Medicine showed an AI system outperforming radiologists in detecting lung cancer on low-dose CT scans — with fewer false positives and false negatives. These tools aren't replacing radiologists; they're acting as a second reader, catching findings that might be missed in a high-volume environment.
The FDA's Digital Health Center of Excellence has cleared over 950 AI/ML-enabled devices, the majority in radiology. This regulatory momentum signals that imaging AI is becoming standard of care.
Predictive analytics and patient risk stratification
Predictive AI models analyze patterns in EHR data — diagnoses, medications, lab values, social determinants — to identify which patients are at elevated risk for deterioration, readmission, or disease progression.
Hospital systems like UCSF and Johns Hopkins have deployed early warning systems that alert clinical teams when hospitalized patients show early signs of sepsis or cardiac decline, hours before the condition becomes obvious. In outpatient settings, AI risk scores help care managers prioritize outreach to high-risk patients before they end up in the ED.
Clinical decision support
Beyond diagnostics and documentation, AI is increasingly embedded at the point of care to support clinical reasoning in real time.
Clinical decision support (CDS) tools surface relevant information, like:
- Drug interactions
- Evidence-based guidelines
- Contraindications
- Diagnostic differentials
Modern AI-powered CDS goes significantly further than the rule-based alert systems that have frustrated clinicians for decades.
Traditional EHR alerts are blunt instruments: they fire constantly, often for obvious reasons, and are overridden 90% of the time. AI-driven CDS learns from the patient's full clinical context and delivers targeted, prioritized recommendations.
In practice, this looks like: an AI flagging that a patient's symptom cluster — mild confusion, elevated creatinine, and recent NSAID use — warrants workup for acute kidney injury before the physician has consciously connected those dots. Or surfacing a newer treatment guideline that changed since the clinician last reviewed that condition. Or prompting a review of a patient's medication list before prescribing a new drug with a non-obvious interaction.
The distinction between AI decision support and AI decision-making matters enormously here. These tools augment clinical judgment. The physician remains accountable for every clinical decision. What AI does is reduce the cognitive load of keeping track of everything, so clinical judgment can focus where it matters most.
Clinical decision support example

Freed has expanded into a clinician assistant — pulling patient details forward, adding visit summaries, and:
- Providing clinical decision support with 50+ verified sources
- Helping you think through A&Ps
- Summarizing key findings with dates
The clinician assistant can be accessed both before and after capturing a visit. You can ask pre-visit questions about a patient you've seen before by clicking the "Ask anything" chat box at the bottom of the screen.
Learn more about Freed’s clinician assistant
Drug discovery and genomics
Drug development is expensive, slow, and failure-prone: it takes an average of 10–15 years and over $2 billion to bring a new drug to market, with a greater than 90% clinical trial failure rate.
AI is compressing that timeline.
Machine learning models can screen millions of molecular compounds in silico, identifying candidates with the highest likelihood of binding to a target protein — work that would take decades in a wet lab.
DeepMind's AlphaFold transformed structural biology by predicting protein structures with near-experimental accuracy, accelerating drug target identification across nearly every disease area.
In genomics, AI is enabling more precise interpretation of whole genome sequencing data, helping clinicians identify rare disease diagnoses that previously went undetected for years.
Administrative automation
The administrative burden in U.S. healthcare is staggering: an estimated $265 billion is wasted annually on administrative complexity. AI is attacking this problem from multiple angles — and some of the most immediate gains are happening at the front desk and on the phones.
These tools often:
- Answer calls
- Support structured intake and scheduling
- Summarize calls and next steps. At the enterprise end of the spectrum, the best AI voice agent platforms can handle the same workflows for high-volume health system contact centers, with sovereign deployment and full audit trails.
See the evolution from traditional front desk to AI reception
Medical reception and front-desk automation
AI-powered virtual receptionists can support call triaging, patient intake, insurance verification, and callback requests around the clock.
For practices with high call volumes, this frees front-desk teams to focus on patients who are physically in the office rather than managing a phone queue.
Phone-based symptom triage
AI triage tools — deployed via phone, patient portal, or SMS — conduct structured symptom interviews and route patients to the appropriate level of care.
A patient calling about chest pain gets a different response than one calling about a medication refill.
AI triage systems trained on clinical protocols can assess urgency, document symptom onset and severity, and either book an appointment at the right time slot, advise self-care, or escalate to a clinical team member for immediate review.
This handles the volume that would otherwise queue up and wait.
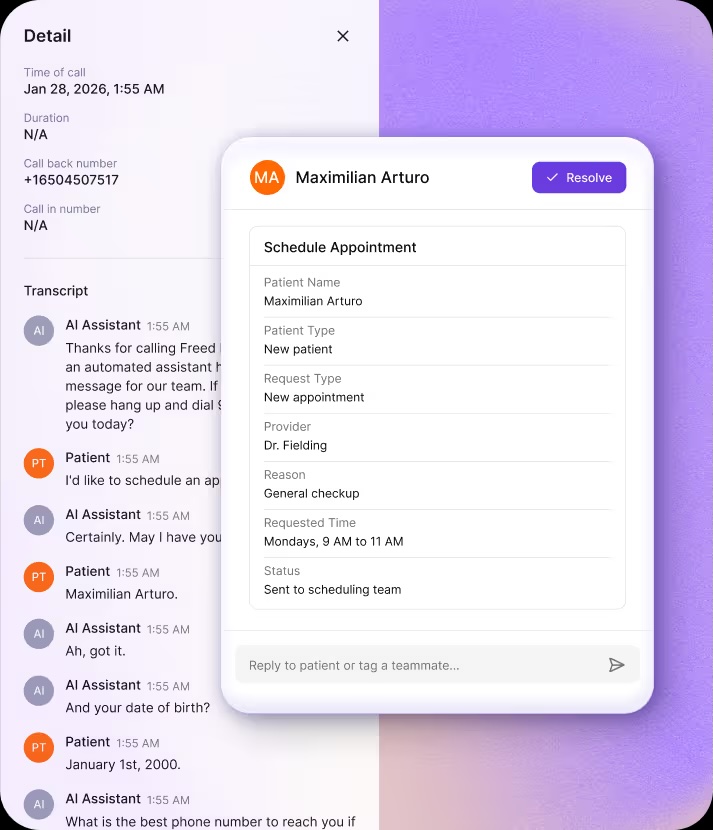
See how Freed Front Desk handles and triages calls 24/7 — plus 2-way SMS messaging
Scheduling optimization
These tools predict no-show rates and patient demand, dynamically filling cancellation slots and reducing idle time. Prior authorization AI can draft and submit authorization requests automatically, flagging cases likely to be denied so staff can intervene early.
Automated coding and billing support
For a large majority of US-based clinicians, billing tasks just add to the admin overload.
It's no surprise: for every visit, you have to choose from 69,000 ICD-10 diagnosis codes and match them to the right CPT codes for procedures. All this has to be done in compliance with payer requirements and documentation guidelines.
Here's another great example of artificial intelligence. With real-time clinical documentation and guidelines, you can properly train artificial intelligence to identify relevant billing codes and make sure every note meets billing requirements.
These tools can also:
- Flag missing elements in reimbursement requests
- Track coding patterns
- Suggest more applicable codes
AI medical coding example
.png)
Freed helps streamline the billing process by identifying relevant ICD-10 diagnosis codes directly from the clinical context of the visit.
As soon as the note is generated, suggested codes appear for review — eliminating the need to manually search through thousands of possible diagnosis codes. These suggestions adapt to the clinician’s specialty and documentation patterns, helping prepare notes for
Real-world examples of AI in healthcare
AI scribes reducing physician documentation burden
The burnout numbers are hard to ignore. The average physician spends 15.5 hours per week on EHR documentation.
Ambient AI scribes represent the most direct, scalable intervention available. Physicians using Freed report a measurable difference not just in time saved, but in how they show up in the exam room. When you're not mentally drafting a note during the visit, you can actually listen.
See how one FQHC saved 12,800 hours in one year with Freed
AI in radiology: FDA-cleared tools
Aidoc, Subtle Medical, Annalise.ai, and Viz.ai are among the companies with FDA-cleared AI tools deployed in hospital radiology departments. Viz.ai's stroke detection software, for example, automatically analyzes CT angiography images and alerts the neurovascular team the moment a large vessel occlusion is detected — shaving critical minutes off time-to-treatment in stroke care.
These tools don't operate autonomously. A radiologist or clinician reviews every AI flag.
AI-assisted coding and claim accuracy
Revenue cycle AI is one of the fastest-growing segments of healthcare AI. Companies like Freed, Cohere Health, Olive, and Infinitus are deploying AI across the claims workflow — from coding assistance at the point of documentation, to prior auth automation, to denial management.
Practices are seeing reduction in claim denials and a meaningful improvement in coder productivity. The economics are straightforward: cleaner claims mean faster reimbursement and less time spent on appeals.
“Unfortunately, in training we just don't learn about coding — but it's the lifeline of everyone's livelihood. With Freed coding assistant, the variability has really tightened. That’s a really positive indicator that our providers are coding at a consistent and standardized level.” — Dr. Boylston, Burlington Pediatrics
Learn more about Freed's coding assistant
Benefits of AI in healthcare
The case for healthcare AI is accumulating in peer-reviewed journals, hospital case studies, and the lived experience of clinicians who've adopted these tools.
Time savings
Ambient AI scribes recover 2+ hours per physician per day. At scale, across a practice or health system, that translates to millions of dollars in recovered capacity.
Reduced burnout
When documentation and admin burden drops, burnout follows. A 2025 JAMA study found that physicians using AI scribing tools reported significantly lower rates of emotional exhaustion after 90 days.
Diagnostic accuracy
In specific, well-defined tasks (reading mammograms, detecting diabetic retinopathy, flagging sepsis), AI has demonstrated performance that matches or exceeds human specialists.
The key word is specific. AI performs best in narrow, high-volume tasks with clear ground truth.
Patient experience
When physicians aren't buried in documentation, they make more eye contact, ask better follow-up questions, and communicate more clearly. Patients notice. Press Ganey data shows a consistent correlation between reduced EHR burden and improved patient satisfaction scores.
Operational efficiency
From scheduling to prior auth to coding, AI reduces the manual overhead that consumes healthcare administration. For independent practices operating on thin margins, this efficiency is existential.
Challenges and ethical considerations
It's easy to be an AI skeptic — there's so much to care about: patient data privacy, HIPAA compliance, and clinical precision.
After all, the stakes are high. A misunderstood medication name, an incorrect diagnosis code, or a data privacy breach can have serious implications.
AI in healthcare is not without real risks. Any honest accounting has to include them.
So, let’s answer some of these questions and address the critical concerns around AI adoption in healthcare.
Algorithmic bias
AI models trained on historical data can perpetuate and amplify the biases embedded in that data. A now-famous study published in Science found that a widely used clinical algorithm systematically underestimated the health needs of Black patients. Ensuring diverse, representative training data is a prerequisite for equitable AI.
Explainability
Many of the most powerful AI models — particularly deep learning systems — are black boxes. They produce outputs without clear explanations of how they arrived at them. In high-stakes clinical decisions, clinicians need to understand the reasoning, not just the recommendation.
Data privacy
Healthcare data is among the most sensitive personal information that exists. Any AI system handling it must meet HIPAA requirements.
Doing that requires more than checking a compliance box. It requires thoughtful data architecture, rigorous access controls, and a genuine commitment to patient privacy.
For example, Freed operates on Microsoft Azure's secure cloud infrastructure and follows strict data management protocols. It doesn’t store any patient recordings and automatically deletes notes after 30 days.
See Freed's data and compliance policies
Overreliance
AI is a tool, not a clinician. The risk of automation bias — the tendency to defer to an AI recommendation even when clinical instinct says otherwise — is real. Training clinicians to use AI as a second opinion, not a final answer, is essential.
Liability
When an AI-assisted diagnosis is wrong, who bears responsibility? The regulatory and legal frameworks around AI liability in healthcare are still developing. Clinicians adopting AI tools should understand what accountability looks like.
Cost and ROI
AI tool adoption can deliver instant returns through time savings and higher efficiency. When you consider the hours saved on documentation alone, you’d see an ROI on your monthly subscription cost for an AI tool. You can even use free trials to discover what a tool brings to the table.
Research suggests that AI scribes have the upper hand when compared to the cost of hiring in-person medical scribes.
“In our study, monthly and initial software costs are $1850/month and $1000 to onboard a clinician. Locally, a scribe costs ∼$3050/month, inclusive of recruiting and training costs. Utilizing DAX over an in-person scribe could equate to ∼$13,400 to ∼$14,400 in cost savings, although additional work that in-person scribes perform (including entering orders or patient instructions) is not possible with DAX. These costs may not be generalizable given our pilot study was performed at a large academic institution.”
Quality control and accuracy
Modern AI tools work on sophisticated large language models (LLMs). These models are designed to achieve remarkable accuracy. They can also learn your specific guidelines and adapt to your preferences over time. As a result, AI tools can reach the highest levels of accuracy.
Besides, think of artificial intelligence as a powerful assistant designed to handle the administrative burden on your behalf. While AI tools do the heavy lifting, you can always review and edit the output for stricter quality control.
This combination of AI efficiency and human oversight promises both speed and accuracy.
Impact on patient relationships
If anything, many clinicians report the opposite. The EHR already pulled clinicians away from patients — AI brings them back. Address privacy worries and ethical concerns upfront, and what's left is a tool that makes you more efficient and more present. Conversations feel like conversations again. That's not a small thing — 81% of clinicians believe that documentation tasks impede patient care.
That's the importance of AI: a chance to be present in the moment on and off the clock.
The future of AI in healthcare (2026 and beyond)
Several trajectories are worth watching closely as AI in healthcare matures.
Multimodal AI
Models will simultaneously process text, imaging, genomic data, and wearable sensor data — is beginning to move from research to clinical validation. The promise: a more holistic, longitudinal view of patient health that no single data source can provide alone.
AI agents
Agents can autonomously complete multi-step clinical or administrative tasks (not just generate a single output) are entering early clinical deployment. Imagine an AI that doesn't just draft a prior auth request, but monitors its status, follows up when needed, and flags the case for human review if denied — without a staff member orchestrating each step.
Freed's CEO unpacks the future of agents and clinical AI
Ambient intelligence at the point of care
This will continue to expand beyond documentation. In the near term, AI systems will passively observe clinical workflows — flagging missed diagnoses, identifying patients due for preventive care, surfacing relevant clinical guidelines during the encounter — without requiring the physician to actively query a system.
Regulatory clarity
This is coming. The FDA's evolving framework for AI/ML-based Software as a Medical Device (SaMD) is maturing, and the EU AI Act will shape how medical AI is developed and deployed globally. Expect more transparency requirements, post-market surveillance mandates, and clearer liability frameworks.
The consensus among healthcare AI researchers: the technology is advancing faster than the institutions, regulations, and clinical cultures designed to govern it. The physicians and practice leaders who engage with these tools thoughtfully — understanding both their power and their limits — will be best positioned to benefit.
How Freed brings AI across the entire practice
Freed started as an ambient AI medical scribe. Today, it's a full clinical operations platform — purpose-built for healthcare, HIPAA-compliant by design, and built around the workflows of real clinicians and practice staff.
Ready to reclaim thousands of clinical hours? Start your free trial — no credit card needed!
Table of Contents
Artificial intelligence (AI) is automating healthcare workflow from end-to-end.
And for good reason: Physicians were spending more time staring at screens than at patients. A study in Annals of Internal Medicine found that physicians spend nearly 2 hours on EHR and desk work for every hour of direct patient care during office hours, plus an additional 1-2 hours nightly on EHR tasks outside work.
From ambient AI scribes that listen to patient visits and write clinical notes in real time, to machine learning algorithms that detect cancer in radiology images before a radiologist can, AI is moving from hype to hands-on clinical utility.
And it's moving at a pace that's hard to overstate. In 2024, the FDA cleared over 950 AI-enabled medical devices.
This guide breaks down what AI in healthcare actually means in 2026 — the technologies, the real-world applications, the benefits, the risks, and what clinicians and practice owners need to know before adopting any of it.
What is AI in healthcare?
Artificial intelligence in healthcare refers to the use of machine learning algorithms, natural language processing, computer vision, and related technologies to:
- Analyze clinical data
- Automate administrative tasks
- Support medical decision-making.
To be perfectly clear: none of these tools can or should replace physicians. They're designed to give back the cognitive bandwidth to do what only you can do: practice medicine.
Healthcare AI spans a wide range. There are chatbots that triage patient symptoms before a visit, eep learning models that flag early-stage diabetic retinopathy in a retinal scan, and ambient microphones that turn a physician-patient conversation into a structured SOAP note.
How AI processes clinical data
AI systems in healthcare are trained on large datasets — medical images, EHR records, clinical notes, genomic sequences, claims data — to identify patterns at scale. The process typically involves three stages:
- Data ingestion: Structured data (lab values, vitals, ICD codes) and unstructured data (clinical notes, imaging, voice recordings) are collected and formatted.
- Model training: Algorithms learn from labeled historical data. For example, thousands of chest X-rays annotated as "pneumonia" or "no finding."
- Inference: The trained model applies what it learned to new, real-world inputs and generates a prediction, recommendation, or output (like a clinical note).
The quality of an AI model is only as good as the data it's trained on — which is why bias, data privacy, and model transparency are central to every responsible healthcare AI deployment.
Key AI technologies used in medicine
Machine learning (ML)
This is the foundational layer of most healthcare AI. ML models find patterns in structured data — predicting which patients are at risk for sepsis, for example, based on lab trends and vital signs.
Natural language processing (NLP)
This enables AI to understand and generate human language. It powers ambient AI scribes that transcribe and structure clinical conversations, as well as tools that extract meaning from unstructured clinical notes.
Computer vision
This allows AI to interpret medical images — X-rays, MRIs, dermatology photos, pathology slides. Models trained on millions of annotated images can now match or exceed specialist-level performance in specific diagnostic tasks.
Generative AI
Now we have the technology behind tools like ChatGPT. It can synthesize, summarize, and generate text. In healthcare, it's being used to draft clinical notes, write after-visit summaries, and produce patient communication — though with important guardrails around accuracy and HIPAA compliance.
Key Applications of AI in Healthcare
When people hear “AI in healthcare,” they often imagine something futuristic — robotic surgeons or fully automated hospitals.
That's far removed from what clinicians actually need: help with the medical documentation, administrative work, and end-to-end workflows.
Here's how AI is making a positive mark for clinics and practitioners.
Clinical documentation and ambient AI scribing
Documentation burden is the highest-ROI application of AI in healthcare today. 77% of pulse survey respondents said that they finish work later than desired or work at home due to medical documentation.
Every patient visit requires clinicians to record key information including:
- Patient history
- Symptoms and exam findings
- Clinical impressions
- Treatment plans
- Follow-up instructions
This patient care documentation tool serves multiple purposes. It supports:
After-hours charting is so common that it's earned a name: "pajama time," ie., catching up on notes at 10 PM after a full day of patients. In fact, 63% of physicians in the US claim to be emotionally exhausted due to burnout.
Ambient AI scribes work by listening to the physician-patient conversation (with patient consent), transcribing it in real time, and generating a structured clinical note. The physician reviews, edits if needed, and approves. What used to take 15 minutes per patient takes two.
Freed's AI scribe, one of the leading ambient tools, supports 100+ specialties, and offers a one-click integration with browser-based EHRs such as athenahealth, eClinicalworks, Practice Fusion, Elation, and more. It also can:
- Carries patient context forward for continuity of care
- Surface ICD-10 and CPT codes with the highest possible E/M ratings
- Supports clinical-decision making with 50+ verified medical sources
- Generates patient letters, referrals, and any other documentation in several languages
.png)
See how Freed builds documentation, codes, and more.
Medical imaging and diagnostics
AI is arguably most mature in radiology and pathology.
FDA-cleared imaging AI tools now assist in reading chest X-rays, detecting breast cancer in mammograms, identifying strokes on CT scans, and flagging diabetic retinopathy in fundus photos.
In 2023, a landmark study published in Nature Medicine showed an AI system outperforming radiologists in detecting lung cancer on low-dose CT scans — with fewer false positives and false negatives. These tools aren't replacing radiologists; they're acting as a second reader, catching findings that might be missed in a high-volume environment.
The FDA's Digital Health Center of Excellence has cleared over 950 AI/ML-enabled devices, the majority in radiology. This regulatory momentum signals that imaging AI is becoming standard of care.
Predictive analytics and patient risk stratification
Predictive AI models analyze patterns in EHR data — diagnoses, medications, lab values, social determinants — to identify which patients are at elevated risk for deterioration, readmission, or disease progression.
Hospital systems like UCSF and Johns Hopkins have deployed early warning systems that alert clinical teams when hospitalized patients show early signs of sepsis or cardiac decline, hours before the condition becomes obvious. In outpatient settings, AI risk scores help care managers prioritize outreach to high-risk patients before they end up in the ED.
Clinical decision support
Beyond diagnostics and documentation, AI is increasingly embedded at the point of care to support clinical reasoning in real time.
Clinical decision support (CDS) tools surface relevant information, like:
- Drug interactions
- Evidence-based guidelines
- Contraindications
- Diagnostic differentials
Modern AI-powered CDS goes significantly further than the rule-based alert systems that have frustrated clinicians for decades.
Traditional EHR alerts are blunt instruments: they fire constantly, often for obvious reasons, and are overridden 90% of the time. AI-driven CDS learns from the patient's full clinical context and delivers targeted, prioritized recommendations.
In practice, this looks like: an AI flagging that a patient's symptom cluster — mild confusion, elevated creatinine, and recent NSAID use — warrants workup for acute kidney injury before the physician has consciously connected those dots. Or surfacing a newer treatment guideline that changed since the clinician last reviewed that condition. Or prompting a review of a patient's medication list before prescribing a new drug with a non-obvious interaction.
The distinction between AI decision support and AI decision-making matters enormously here. These tools augment clinical judgment. The physician remains accountable for every clinical decision. What AI does is reduce the cognitive load of keeping track of everything, so clinical judgment can focus where it matters most.
Clinical decision support example

Freed has expanded into a clinician assistant — pulling patient details forward, adding visit summaries, and:
- Providing clinical decision support with 50+ verified sources
- Helping you think through A&Ps
- Summarizing key findings with dates
The clinician assistant can be accessed both before and after capturing a visit. You can ask pre-visit questions about a patient you've seen before by clicking the "Ask anything" chat box at the bottom of the screen.
Learn more about Freed’s clinician assistant
Drug discovery and genomics
Drug development is expensive, slow, and failure-prone: it takes an average of 10–15 years and over $2 billion to bring a new drug to market, with a greater than 90% clinical trial failure rate.
AI is compressing that timeline.
Machine learning models can screen millions of molecular compounds in silico, identifying candidates with the highest likelihood of binding to a target protein — work that would take decades in a wet lab.
DeepMind's AlphaFold transformed structural biology by predicting protein structures with near-experimental accuracy, accelerating drug target identification across nearly every disease area.
In genomics, AI is enabling more precise interpretation of whole genome sequencing data, helping clinicians identify rare disease diagnoses that previously went undetected for years.
Administrative automation
The administrative burden in U.S. healthcare is staggering: an estimated $265 billion is wasted annually on administrative complexity. AI is attacking this problem from multiple angles — and some of the most immediate gains are happening at the front desk and on the phones.
These tools often:
- Answer calls
- Support structured intake and scheduling
- Summarize calls and next steps. At the enterprise end of the spectrum, the best AI voice agent platforms can handle the same workflows for high-volume health system contact centers, with sovereign deployment and full audit trails.
See the evolution from traditional front desk to AI reception
Medical reception and front-desk automation
AI-powered virtual receptionists can support call triaging, patient intake, insurance verification, and callback requests around the clock.
For practices with high call volumes, this frees front-desk teams to focus on patients who are physically in the office rather than managing a phone queue.
Phone-based symptom triage
AI triage tools — deployed via phone, patient portal, or SMS — conduct structured symptom interviews and route patients to the appropriate level of care.
A patient calling about chest pain gets a different response than one calling about a medication refill.
AI triage systems trained on clinical protocols can assess urgency, document symptom onset and severity, and either book an appointment at the right time slot, advise self-care, or escalate to a clinical team member for immediate review.
This handles the volume that would otherwise queue up and wait.

See how Freed Front Desk handles and triages calls 24/7 — plus 2-way SMS messaging
Scheduling optimization
These tools predict no-show rates and patient demand, dynamically filling cancellation slots and reducing idle time. Prior authorization AI can draft and submit authorization requests automatically, flagging cases likely to be denied so staff can intervene early.
Automated coding and billing support
For a large majority of US-based clinicians, billing tasks just add to the admin overload.
It's no surprise: for every visit, you have to choose from 69,000 ICD-10 diagnosis codes and match them to the right CPT codes for procedures. All this has to be done in compliance with payer requirements and documentation guidelines.
Here's another great example of artificial intelligence. With real-time clinical documentation and guidelines, you can properly train artificial intelligence to identify relevant billing codes and make sure every note meets billing requirements.
These tools can also:
- Flag missing elements in reimbursement requests
- Track coding patterns
- Suggest more applicable codes
AI medical coding example
.png)
Freed helps streamline the billing process by identifying relevant ICD-10 diagnosis codes directly from the clinical context of the visit.
As soon as the note is generated, suggested codes appear for review — eliminating the need to manually search through thousands of possible diagnosis codes. These suggestions adapt to the clinician’s specialty and documentation patterns, helping prepare notes for
Real-world examples of AI in healthcare
AI scribes reducing physician documentation burden
The burnout numbers are hard to ignore. The average physician spends 15.5 hours per week on EHR documentation.
Ambient AI scribes represent the most direct, scalable intervention available. Physicians using Freed report a measurable difference not just in time saved, but in how they show up in the exam room. When you're not mentally drafting a note during the visit, you can actually listen.
See how one FQHC saved 12,800 hours in one year with Freed
AI in radiology: FDA-cleared tools
Aidoc, Subtle Medical, Annalise.ai, and Viz.ai are among the companies with FDA-cleared AI tools deployed in hospital radiology departments. Viz.ai's stroke detection software, for example, automatically analyzes CT angiography images and alerts the neurovascular team the moment a large vessel occlusion is detected — shaving critical minutes off time-to-treatment in stroke care.
These tools don't operate autonomously. A radiologist or clinician reviews every AI flag.
AI-assisted coding and claim accuracy
Revenue cycle AI is one of the fastest-growing segments of healthcare AI. Companies like Freed, Cohere Health, Olive, and Infinitus are deploying AI across the claims workflow — from coding assistance at the point of documentation, to prior auth automation, to denial management.
Practices are seeing reduction in claim denials and a meaningful improvement in coder productivity. The economics are straightforward: cleaner claims mean faster reimbursement and less time spent on appeals.
“Unfortunately, in training we just don't learn about coding — but it's the lifeline of everyone's livelihood. With Freed coding assistant, the variability has really tightened. That’s a really positive indicator that our providers are coding at a consistent and standardized level.” — Dr. Boylston, Burlington Pediatrics
Learn more about Freed's coding assistant
Benefits of AI in healthcare
The case for healthcare AI is accumulating in peer-reviewed journals, hospital case studies, and the lived experience of clinicians who've adopted these tools.
Time savings
Ambient AI scribes recover 2+ hours per physician per day. At scale, across a practice or health system, that translates to millions of dollars in recovered capacity.
Reduced burnout
When documentation and admin burden drops, burnout follows. A 2025 JAMA study found that physicians using AI scribing tools reported significantly lower rates of emotional exhaustion after 90 days.
Diagnostic accuracy
In specific, well-defined tasks (reading mammograms, detecting diabetic retinopathy, flagging sepsis), AI has demonstrated performance that matches or exceeds human specialists.
The key word is specific. AI performs best in narrow, high-volume tasks with clear ground truth.
Patient experience
When physicians aren't buried in documentation, they make more eye contact, ask better follow-up questions, and communicate more clearly. Patients notice. Press Ganey data shows a consistent correlation between reduced EHR burden and improved patient satisfaction scores.
Operational efficiency
From scheduling to prior auth to coding, AI reduces the manual overhead that consumes healthcare administration. For independent practices operating on thin margins, this efficiency is existential.
Challenges and ethical considerations
It's easy to be an AI skeptic — there's so much to care about: patient data privacy, HIPAA compliance, and clinical precision.
After all, the stakes are high. A misunderstood medication name, an incorrect diagnosis code, or a data privacy breach can have serious implications.
AI in healthcare is not without real risks. Any honest accounting has to include them.
So, let’s answer some of these questions and address the critical concerns around AI adoption in healthcare.
Algorithmic bias
AI models trained on historical data can perpetuate and amplify the biases embedded in that data. A now-famous study published in Science found that a widely used clinical algorithm systematically underestimated the health needs of Black patients. Ensuring diverse, representative training data is a prerequisite for equitable AI.
Explainability
Many of the most powerful AI models — particularly deep learning systems — are black boxes. They produce outputs without clear explanations of how they arrived at them. In high-stakes clinical decisions, clinicians need to understand the reasoning, not just the recommendation.
Data privacy
Healthcare data is among the most sensitive personal information that exists. Any AI system handling it must meet HIPAA requirements.
Doing that requires more than checking a compliance box. It requires thoughtful data architecture, rigorous access controls, and a genuine commitment to patient privacy.
For example, Freed operates on Microsoft Azure's secure cloud infrastructure and follows strict data management protocols. It doesn’t store any patient recordings and automatically deletes notes after 30 days.
See Freed's data and compliance policies
Overreliance
AI is a tool, not a clinician. The risk of automation bias — the tendency to defer to an AI recommendation even when clinical instinct says otherwise — is real. Training clinicians to use AI as a second opinion, not a final answer, is essential.
Liability
When an AI-assisted diagnosis is wrong, who bears responsibility? The regulatory and legal frameworks around AI liability in healthcare are still developing. Clinicians adopting AI tools should understand what accountability looks like.
Cost and ROI
AI tool adoption can deliver instant returns through time savings and higher efficiency. When you consider the hours saved on documentation alone, you’d see an ROI on your monthly subscription cost for an AI tool. You can even use free trials to discover what a tool brings to the table.
Research suggests that AI scribes have the upper hand when compared to the cost of hiring in-person medical scribes.
“In our study, monthly and initial software costs are $1850/month and $1000 to onboard a clinician. Locally, a scribe costs ∼$3050/month, inclusive of recruiting and training costs. Utilizing DAX over an in-person scribe could equate to ∼$13,400 to ∼$14,400 in cost savings, although additional work that in-person scribes perform (including entering orders or patient instructions) is not possible with DAX. These costs may not be generalizable given our pilot study was performed at a large academic institution.”
Quality control and accuracy
Modern AI tools work on sophisticated large language models (LLMs). These models are designed to achieve remarkable accuracy. They can also learn your specific guidelines and adapt to your preferences over time. As a result, AI tools can reach the highest levels of accuracy.
Besides, think of artificial intelligence as a powerful assistant designed to handle the administrative burden on your behalf. While AI tools do the heavy lifting, you can always review and edit the output for stricter quality control.
This combination of AI efficiency and human oversight promises both speed and accuracy.
Impact on patient relationships
If anything, many clinicians report the opposite. The EHR already pulled clinicians away from patients — AI brings them back. Address privacy worries and ethical concerns upfront, and what's left is a tool that makes you more efficient and more present. Conversations feel like conversations again. That's not a small thing — 81% of clinicians believe that documentation tasks impede patient care.
That's the importance of AI: a chance to be present in the moment on and off the clock.
The future of AI in healthcare (2026 and beyond)
Several trajectories are worth watching closely as AI in healthcare matures.
Multimodal AI
Models will simultaneously process text, imaging, genomic data, and wearable sensor data — is beginning to move from research to clinical validation. The promise: a more holistic, longitudinal view of patient health that no single data source can provide alone.
AI agents
Agents can autonomously complete multi-step clinical or administrative tasks (not just generate a single output) are entering early clinical deployment. Imagine an AI that doesn't just draft a prior auth request, but monitors its status, follows up when needed, and flags the case for human review if denied — without a staff member orchestrating each step.
Freed's CEO unpacks the future of agents and clinical AI
Ambient intelligence at the point of care
This will continue to expand beyond documentation. In the near term, AI systems will passively observe clinical workflows — flagging missed diagnoses, identifying patients due for preventive care, surfacing relevant clinical guidelines during the encounter — without requiring the physician to actively query a system.
Regulatory clarity
This is coming. The FDA's evolving framework for AI/ML-based Software as a Medical Device (SaMD) is maturing, and the EU AI Act will shape how medical AI is developed and deployed globally. Expect more transparency requirements, post-market surveillance mandates, and clearer liability frameworks.
The consensus among healthcare AI researchers: the technology is advancing faster than the institutions, regulations, and clinical cultures designed to govern it. The physicians and practice leaders who engage with these tools thoughtfully — understanding both their power and their limits — will be best positioned to benefit.
How Freed brings AI across the entire practice
Freed started as an ambient AI medical scribe. Today, it's a full clinical operations platform — purpose-built for healthcare, HIPAA-compliant by design, and built around the workflows of real clinicians and practice staff.
Ready to reclaim thousands of clinical hours? Start your free trial — no credit card needed!
FAQs
Frequently asked questions from clinicians and medical practitioners.


